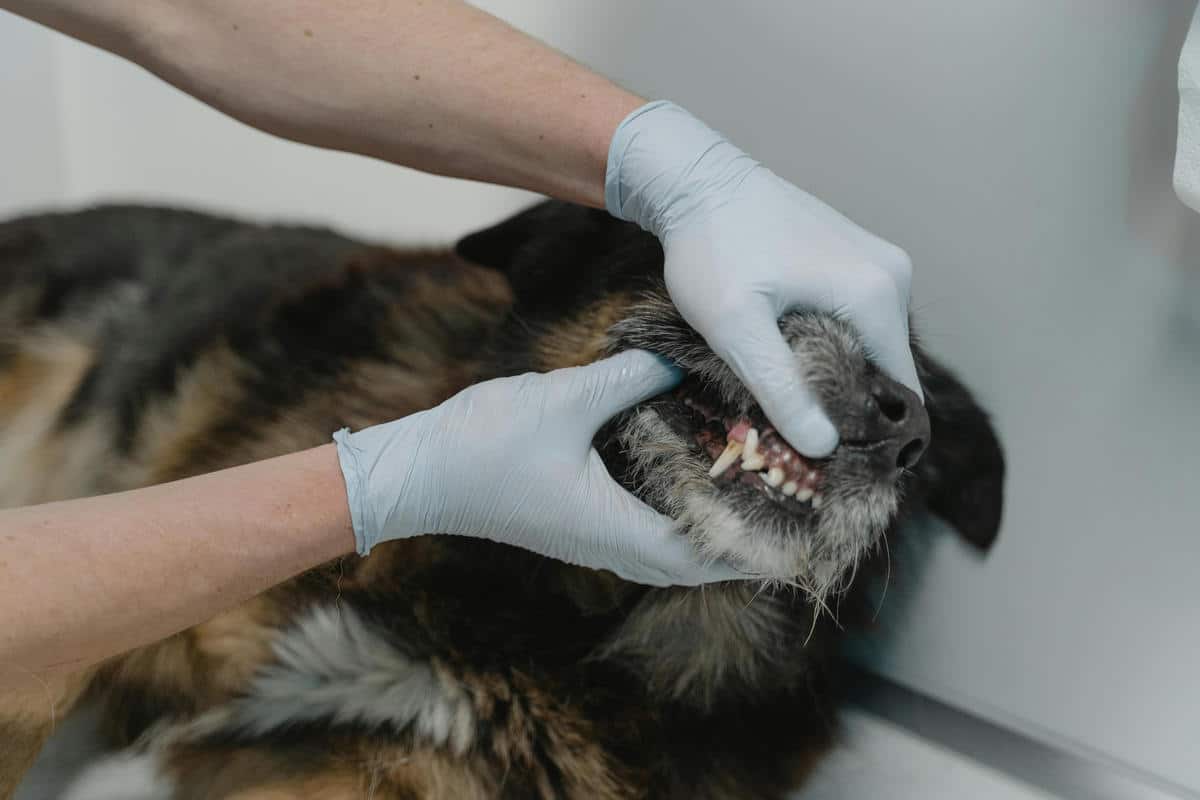
A structured, first-opinion veterinary approach to assessing reduced appetite in small animal practice, focusing on clinical reasoning and diagnostic evaluation.
What you will learn in this article
- How to define and interpret reduced appetite in small animal patients.
- How to distinguish inappetence from true anorexia in clinical practice.
- Which history and examination findings are most diagnostically useful.
- How to organize differential diagnoses using a problem-oriented framework.
- When monitoring is appropriate and when escalation is required.
Defining the Clinical Problem
Reduced appetite is one of the most common presenting complaints in small animal practice. Despite its frequency, it represents a non-specific clinical sign rather than a diagnosis. The first clinical task is therefore to define the problem accurately in the individual patient before considering further investigation.
In everyday consultations, the statement “the patient is not eating” may describe very different clinical situations. Some patients show only a mild reduction in food intake, while others completely refuse all forms of food. These differences are clinically important because they influence both urgency and the subsequent diagnostic approach.
Inappetence
Inappetence refers to a partial reduction in appetite. The patient may eat smaller amounts than normal, become selective about food, or refuse the usual diet while still accepting alternative or highly palatable options. In small animal practice, inappetence is commonly associated with mild gastrointestinal disturbance, early systemic disease, stress-related factors, or recent changes in diet or environment.
The presence of inappetence indicates that some willingness to eat remains. In stable patients, this distinction may allow for short-term monitoring, provided that clear reassessment criteria are established.
Anorexia
Anorexia describes a complete refusal of food. Affected patients show little or no interest in eating, even when offered highly palatable options. Clinically, anorexia is more concerning than inappetence and is more often associated with significant pain, systemic illness, inflammatory disease, or marked metabolic disturbance.
Why this distinction matters
Correctly differentiating between inappetence and anorexia improves early clinical decision-making. Patients with true anorexia generally warrant a lower threshold for diagnostic investigation and closer monitoring than those with mild inappetence. Failure to make this distinction can lead to delayed recognition of serious underlying disease.
Common pitfall
Do not accept “not eating” as a final description. Always clarify how much food is consumed, what types of food are refused or accepted, and whether the problem represents inappetence or true anorexia.
Once the nature of the appetite abnormality has been clearly defined, the next step is to obtain a focused and purposeful history.
Targeted History Taking
Once reduced appetite has been clearly defined, the next step is to obtain a focused and purposeful history. At this stage, the goal is not to reach a definitive diagnosis, but to narrow the list of likely causes and identify patients that may require urgent investigation.
A common error in small animal practice is asking numerous unfocused questions. Instead, history taking should concentrate on key areas that are most relevant to appetite loss and that provide the greatest diagnostic value.
Duration and onset
Establishing when the appetite change began is essential. Acute onset over hours to a few days is often associated with gastrointestinal upset, dietary indiscretion, acute pain, or stress-related events. In contrast, a chronic or progressively worsening reduction in appetite raises concern for systemic disease, chronic pain, metabolic disorders, or neoplastic processes.
It is also important to determine whether the change was sudden or gradual, as gradual appetite loss is frequently under-recognized by owners and may indicate a longer-standing disease process.
Changes in eating behaviour
Owners may report that the patient is not eating, but careful questioning often reveals more specific patterns. Some patients refuse their normal diet while still accepting treats or hand-fed food, whereas others show little interest in any type of food.
Clarifying what the patient will eat, how eagerly it approaches food, and whether feeding behaviour has changed can provide important diagnostic clues. Selective eating may suggest palatability issues, stress, or early disease, while complete food refusal is more concerning.
Associated clinical signs
Reduced appetite rarely occurs in isolation. The clinician should actively ask about additional signs such as vomiting, diarrhoea, weight loss, lethargy, coughing, changes in drinking or urination, and alterations in behaviour. These associated signs often help direct the diagnostic approach more effectively than appetite loss alone.
Dietary, environmental, and medication history
Recent dietary changes, access to table scraps, scavenging behaviour, or changes in feeding routine should be explored. Environmental factors such as travel, boarding, household changes, or stressors may also contribute to appetite reduction, particularly in cats.
A complete medication history is essential, including recently started treatments and over-the-counter products. Some medications can reduce appetite directly or cause gastrointestinal discomfort that discourages eating.
Assessment of pain
Subtle indicators of pain should always be considered during history taking. Reluctance to move, stiffness, changes in posture, or avoidance of the food bowl may suggest musculoskeletal or oral pain rather than primary gastrointestinal disease.
Clinical tip
A structured history often narrows the differential diagnosis significantly before physical examination or diagnostic testing is performed.
Information obtained during history taking should always be interpreted alongside the findings of a thorough physical examination.
Physical Examination Priorities
The physical examination is a critical component of evaluating reduced appetite in small animal patients. Findings at this stage often help determine whether the problem is likely to be local, systemic, or pain-related and guide the need for further investigation.
The aim is not to perform an exhaustive examination of every system, but to focus on areas most commonly associated with appetite loss while remaining alert to unexpected findings.
General appearance and demeanor
Observation should begin as soon as the patient enters the consultation area. Level of alertness, posture, willingness to move, and interaction with the environment provide valuable information about overall health status.
A bright, responsive patient with mild inappetence may be approached differently from a dull or depressed patient with true anorexia or additional systemic signs.
Body condition and weight
Body condition score and muscle mass should be assessed whenever possible. Even subtle weight loss or muscle wasting may indicate a longer-standing problem than initially reported by the owner.
Oral cavity examination
Examination of the oral cavity is essential in patients with reduced appetite. Dental disease, oral inflammation, fractured teeth, foreign material, or oral masses can all cause pain that discourages eating.
Patients with oral pain may approach food but then drop it, chew on one side, or walk away from the food bowl. These signs may be missed if the oral cavity is not examined carefully.
Abdominal palpation
Gentle abdominal palpation should be performed to assess for pain, distension, masses, or abnormal organ size. Gastrointestinal discomfort is a common cause of appetite loss, and localized pain may help guide further diagnostic steps.
Marked abdominal pain, guarding, or distension should be considered significant findings and may warrant prompt diagnostic evaluation.
Hydration status and body temperature
Assessment of hydration status provides insight into disease severity and duration. Dehydration may reflect reduced intake, ongoing fluid losses, or systemic illness.
Body temperature should always be recorded. Fever supports an inflammatory or infectious process, while hypothermia in an unwell patient is a concerning indicator of systemic compromise.
Lymph nodes and musculoskeletal system
Peripheral lymph nodes should be palpated routinely. Generalized lymphadenopathy may suggest systemic disease, while localized enlargement may indicate regional pathology.
The musculoskeletal system should not be overlooked. Pain associated with joints, spine, or movement can reduce appetite, particularly in older patients.
Clinical reminder
Reduced appetite is frequently secondary to pain. A normal gastrointestinal examination does not exclude musculoskeletal, oral, or systemic causes.
Findings from the physical examination should be integrated with the history to determine whether monitoring, targeted diagnostics, or immediate escalation is most appropriate.
Differential Diagnosis Framework
Following history taking and physical examination, potential causes of reduced appetite should be organized into a logical differential diagnosis framework. At this stage, the objective is not to identify a single definitive diagnosis, but to group possibilities in a structured way that guides further investigation.
Using a problem-oriented framework helps avoid common diagnostic errors, such as focusing too early on gastrointestinal disease or overlooking systemic and pain-related causes.
Gastrointestinal disease
Gastrointestinal conditions are frequently considered when appetite is reduced. Acute gastritis, enteritis, dietary indiscretion, foreign material, or inflammatory bowel disease may all reduce appetite due to nausea or abdominal discomfort.
The presence of vomiting, diarrhoea, abdominal pain, or changes in stool quality increases suspicion of a primary gastrointestinal cause.
Systemic and metabolic disorders
Many systemic diseases are associated with reduced appetite. Renal disease, hepatic disease, endocrine disorders, and chronic inflammatory conditions commonly present with appetite changes as part of a broader clinical picture.
In these cases, appetite loss is often accompanied by lethargy, weight loss, changes in drinking behaviour, or poor body condition.
Pain-related causes
Pain is a frequently under-recognized cause of reduced appetite in small animal patients. Dental disease, oral pathology, musculoskeletal pain, spinal discomfort, or intra-abdominal pain may all discourage eating.
Patients in pain may appear otherwise bright but show subtle changes in posture, movement, or feeding behaviour that point away from primary gastrointestinal disease.
Infectious and inflammatory conditions
Infectious and inflammatory processes often lead to appetite reduction as part of a systemic response. Fever, lymphadenopathy, or other signs of inflammation support consideration of this category.
Appetite loss associated with infection or inflammation is rarely an isolated finding and should prompt further assessment.
Neoplastic disease
Neoplasia should be considered, particularly in older patients or those with chronic, progressive appetite loss and weight loss. Although reduced appetite alone is non-specific, its presence alongside other concerning signs warrants inclusion of neoplastic disease in the differential list.
Clinical approach
Grouping differential diagnoses into broad categories ensures that important causes are not overlooked and provides a rational basis for selecting diagnostic tests.
Once a working list of differential diagnoses has been established, the clinician can determine whether immediate diagnostic testing is required or whether short-term monitoring is appropriate.
Initial Diagnostic Approach
Once a structured differential diagnosis framework has been established, the clinician must decide on an appropriate initial diagnostic approach. Not every patient with reduced appetite requires immediate extensive testing, and the decision should be guided by clinical findings, duration of signs, and overall patient stability.
A common mistake at this stage is either performing excessive testing too early or delaying investigation in patients that clearly warrant further assessment. A rational, stepwise approach helps balance these risks.
Patients suitable for short-term monitoring
In selected cases, a brief period of monitoring may be appropriate. These patients are typically bright, alert, and systemically stable, with mild inappetence of short duration and no concerning abnormalities on physical examination.
When monitoring is chosen, owners should be given clear instructions regarding what changes to observe and when reassessment is required. Monitoring should always be time-limited and purposeful.
Indications for baseline diagnostic testing
Baseline diagnostic testing should be considered when appetite reduction persists, when additional clinical signs are present, or when physical examination findings raise concern for systemic or significant disease.
Initial investigations are most useful when they are selected to address specific clinical questions rather than performed as routine panels. Even limited testing can provide valuable information that guides further decision-making.
Guiding test selection using clinical findings
Results of history taking and physical examination should guide which diagnostic tests are prioritized. Findings suggestive of gastrointestinal disease, systemic illness, or pain-related conditions will influence the choice and sequence of investigations.
This targeted approach reduces unnecessary testing and helps ensure that diagnostic efforts remain focused, efficient, and cost-effective.
The importance of reassessment
Reassessment is a critical component of managing patients with reduced appetite. Patients that fail to improve, develop new clinical signs, or show worsening appetite reduction should be re-evaluated promptly.
Clinical caution
Persistence or progression of reduced appetite despite initial monitoring should prompt escalation of diagnostics to avoid delayed recognition of serious underlying disease.
Following the initial diagnostic approach, the clinician must also be able to recognize situations where more urgent action is required.
Red Flags and When to Escalate
Although many cases of reduced appetite can be approached methodically, certain findings should immediately raise concern. Recognizing these red flags is essential to avoid delays in diagnosing serious or potentially life-threatening conditions.
Persistent anorexia
Complete refusal of food that persists beyond a short period is a significant concern, particularly when accompanied by lethargy or signs of discomfort. Persistent anorexia increases the risk of metabolic complications and is often associated with systemic or severe underlying disease.
Progressive weight loss or poor body condition
Documented weight loss, muscle wastage, or declining body condition score suggests a chronic or progressive process. These findings should lower the threshold for diagnostic testing even if other clinical signs appear mild.
Evidence of systemic illness
Signs such as fever, dehydration, jaundice, marked lethargy, or changes in drinking and urination patterns indicate systemic involvement. Reduced appetite in these patients is rarely an isolated problem and warrants prompt investigation.
High-risk patients
Young animals, geriatric patients, and those with known chronic disease have reduced physiological reserves. Appetite loss in these groups should be approached cautiously, as deterioration may occur more rapidly.
Failure to respond to initial management
Lack of improvement or clinical deterioration during a period of monitoring should prompt reassessment. Failure to respond as expected often indicates that further investigation is required.
Key point
When red flags are present, early escalation of diagnostics is preferable to delayed recognition of serious disease.
Once urgent cases have been identified and addressed, effective communication with the owner becomes essential to ensure appropriate follow-up and compliance.
Communicating With the Owner
Clear and effective communication with the owner is a critical part of managing reduced appetite in small animal practice. Appetite loss often causes significant concern, even when the patient appears otherwise stable, and the clinician plays an important role in guiding expectations and decision-making.
Explaining the clinical problem
Owners frequently expect a single, definitive explanation for why their animal is not eating. It is important to explain that reduced appetite is a non-specific clinical sign and that multiple conditions may produce similar presentations.
Using simple, non-technical language and summarizing key examination findings helps owners understand what has been assessed and what remains uncertain.
Discussing monitoring and uncertainty
When immediate diagnostic testing is not indicated, owners should be given a clear explanation of why short-term monitoring is appropriate. Emphasizing that monitoring is an active process rather than inaction helps build trust.
Uncertainty is an inevitable part of clinical practice, and acknowledging this openly often improves owner confidence and cooperation.
Setting clear follow-up expectations
Owners should leave the consultation with specific guidance on what changes to monitor at home, including appetite, activity level, vomiting, diarrhoea, and weight changes.
Clear instructions regarding when to return for reassessment reduce the risk of delayed presentation in patients whose condition is worsening.
Clinical communication tip
Clear explanations and defined follow-up plans improve owner compliance and reduce the likelihood of missed clinical deterioration.
Effective communication ensures that clinical reasoning is understood and supported, forming an essential link between assessment, monitoring, and ongoing care.
Educational disclaimer:This article is intended for veterinary education and clinical reasoning support only and does not replace professional judgment or case-specific diagnostic evaluation.





























![Ettinger’s Textbook of Veterinary Internal Medicine 9th Edition Ettinger’s Textbook of Veterinary Internal Medicine 9th Edition [True PDF+Videos]](https://www.vet-ebooks.com/wp-content/uploads/2024/10/ettingers-textbook-of-veterinary-internal-medicine-9th-edition-100x70.jpg)



